Photo by Diana Polekhina on Unsplash.
Needle phobia is an overlooked health concern. Needle injections are among the most used medical techniques worldwide for the delivery of therapeutics and preventive care. In fact, one person receives on average 2 to 11 needle injections per year [1]. Needles are used not only for injections but also for blood transfusion and surgery. Thus, needle procedures play a crucial role in healthcare. However, the use of needles in medical procedures is often not well accepted, especially by people that have needle fear or needle phobia.
Needle fear is not the same as needle phobia. Needle fear refers to the anxiety and avoidance of procedures that use needles. Needle phobia is defined as a psychiatric disorder which is anxiety out of proportion to the threat according to the Diagnostic and Statistical Manual of Mental Disorders [2], This condition is caused by a vasovagal response, often diphasic, and can result in serious consequences such as respiratory disturbances, fainting, and even death [1, 3]. These patients can be extremely hard to manage when they need to undergo needle procedures because they are usually misunderstood. If the healthcare professional managing the patient is not properly trained or educated on the subject, accidents can occur.
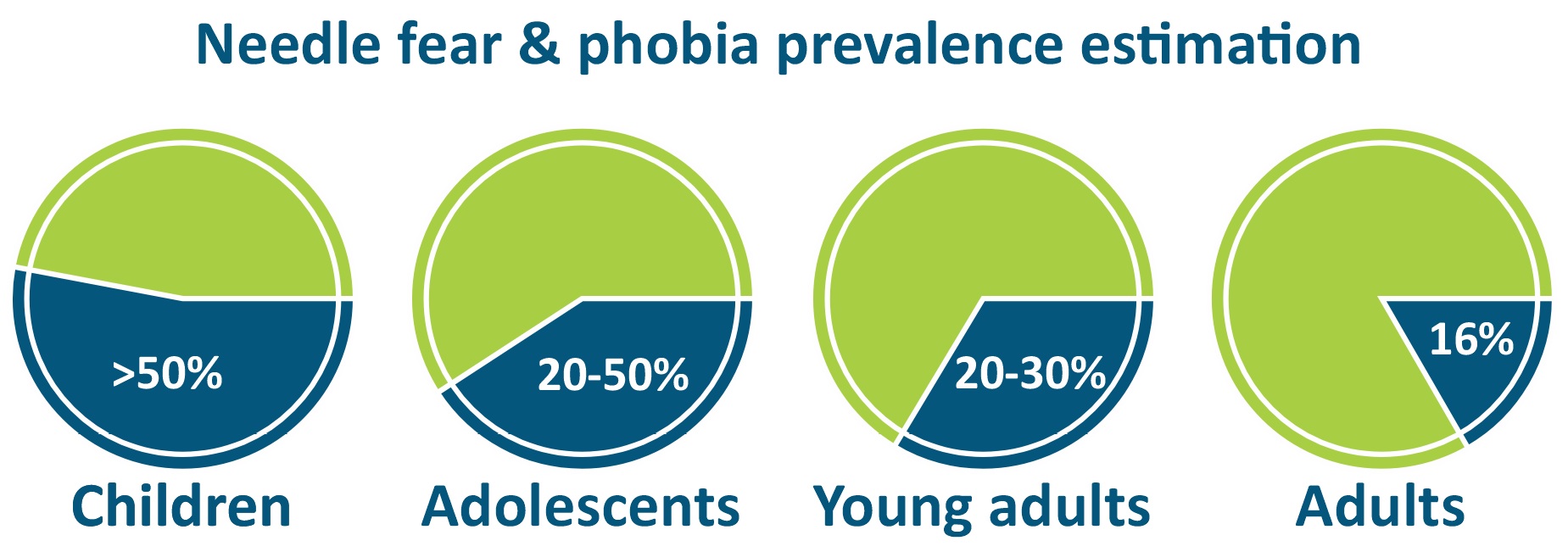
In 1995, it was initially estimated that 10% of the general population present needle phobia [3]. Nowadays, the prevalence estimation diverges considerably between the studies, ranging from 3.5% to 20% and consider both needle fear and needle phobia all together [4]. A systematic review and meta‐analysis were recently performed to obtain more complete estimations of needle fear prevalence. Consistently with other studies [5, 6], it showed that the condition decreased with age and was more common in females than males. The prevalence was estimated to be 16% in adult patients, 20–30% in young adults, 20‐50% in adolescents and more than 50% for children [1].
Additionally, needle phobia is very common in specific health conditions or procedures that require chronic exposure to needles such as cancer undergoing chemotherapy patients, individuals with diabetes and people undergoing routine dental procedures [1]. Accordingly, managing needle phobic Type 1 diabetes mellitus patients for example, can be very challenging [7].
Needle phobia can have serious immediate health consequences as briefly described before. However, one particular concern is that these patients often avoid all procedures that involve needles, even to the detriment of their own health. The condition can be either inherited or acquired through bad experiences [3]. Early experiences with needle procedures can make a difference in whether the patients will seek medical help in the future or not. Obviously, this will also negatively influence the diagnosis of cases since this group usually stay away from healthcare [8].
The condition furthermore impacts a person’s legal and social life [3]. In fact, even self-help books have been published to help the needle fear group to cope with the problem [9]. Public health can also be impacted by needle phobia. Consider vaccinations, one of the most important interventions in public health, often rely on needle injection delivery. Indeed, Love et al discuss the importance of considering needle phobia among adult patients during mass COVID-19 vaccinations [4].
The acknowledge and education about needle phobia and how to spot its victims is key in the combat of this condition. It started to gain attention after it was officially classified as a phobia, incidents were reported, and its etiology and consequences were better defined [3]. Yet, a small part of the general population nor healthcare professionals is fully aware of the condition and few therapeutic alternatives that had sustained benefits were available [4].
Needle fear and phobia can define a person’s engagement with healthcare system and therefore the appropriate management of this condition can save lives [8].
With the advances in technology, innovative solutions to needle fear and phobia started to be explored. Needle-free systems such as oral or nasal vaccines perfectly demonstrate an effective alternative that allows this group to receive healthcare despite the condition. However, many drugs cannot be delivered by these solutions.
Also, novel injection platforms were recently developed. VAX-ID® is an award-winning medical device developed by IDEVAX for accurate intradermal injections. The device can contribute to needle fear or needle phobia patients because it contains a mini-needle which is non-visible to the patient and elicits little or no pain during the injection since the needle enters max 1mm in the patient’s skin. Therefore, VAX-ID® can increase needle fear patient compliance to treatments that require needle injection drug delivery.
References:
- McLenon, Jennifer, and Mary AM Rogers. “The fear of needles: A systematic review and meta‐analysis.” Journal of advanced nursing 75.1 (2019): 30-42.
- American Psychiatric Association. The Diagnostic and Statistical Manual of Mental Disorders: DSM 5. American Psychiatric Association. 2013.
- Hamilton, James G. “Needle phobia: a neglected diagnosis.” Journal of Family Practice 41.2 (1995): 169-182.
- Love, Ashley S., and Robert J. Love. “Considering needle phobia among adult patients during mass COVID-19 vaccinations.” Journal of Primary Care & Community Health 12 (2021): 21501327211007393.
- Taddio, Anna, et al. “Survey of the prevalence of immunization non-compliance due to needle fears in children and adults.” Vaccine 30.32 (2012): 4807-4812.
- Nir, Yael, et al. “Fear of injections in young adults: prevalence and associations.” The American journal of tropical medicine and hygiene 68.3 (2003): 341-344.
- Zambanini, A., and M. D. Feher. “Needle phobia in type 1 diabetes mellitus.” Diabetic Medicine 14.4 (1997): 321-323.
- Jenkins, K. “II. Needle phobia: a psychological perspective.” British journal of anaesthesia 113.1 (2014): 4-6.
- Not OK With Needles? : What to do when a fear of needles is getting in the way of your life: ROSE STEWART: 9781009065627: hive.co.uk. (accessed May 2022).
Interested in our solutions?
Contact our commercial team!
